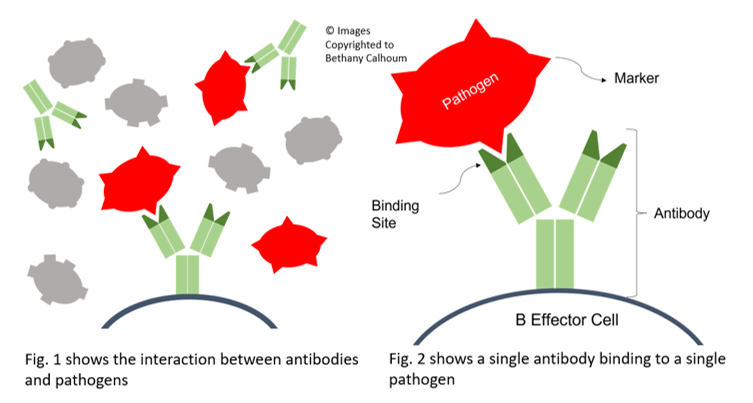
You’ve probably heard that most of the immune system is found in the gut or at least that the gut trains immune function, but you may not know how.
We thought we’d pop together a brief guide to GALT or gut associated lymphoid tissue and how we can use nutrition to optimise it’s function.
GALT stands for gut associated lymphoid tissue and is another subcategory of mucosa-associated lymphoid tissue. GALT is present throughout the lining of the intestine. It consists of a large population of plasma cells and makes up about 70% of the immune system by weight.
Being so close to the microbiome and in immediate contact with food, GALT is continually exposed to both ‘normal’ and potentially dangerous antigens.
This means that GALT develops in a manner that allows non-pathogenic substances, such as commensal bacteria, to survive and enables tolerance to food antigens, whilst at the same time it protects the host from pathogenic organisms and other potentially toxic substances.
In short, GALT matures through exposure, based on this idea of immune tolerance.
Do We Need To Boost Our Pet’s Immunity?
This distinctive biological feature of GALT is believed to be crucial to good health. Deregulation or dysfunction of GALT is thought to predispose to inflammatory bowel diseases (IBD) and more.
The gut microbiota plays an important role in the development of the normal mucosal immune system (humoral and cellular), including the development of gut-associated lymphoid tissues.
Under normal physiological conditions, symbiotic association of gut microbiota with gut-associated lymphoid tissue (GALT) contributes to immune balance.
Dysbiosis continuously and adversely agitates GALT to promote sterile inflammatory response and sensitises the host for chronic gastric disease. There is increasing evidence that suggests changes in intestinal microbiota results in changes in the intercellular tight junctions.
In addition, evidence suggests that dysbiosis is associated with inflammatory bowel disease through its influence on GALT.
Diet and geographical location play a major role in determining the microbial diversity in the gut.
In addition, uncontrolled use of antibiotics also (both prescribed and indiscriminate usage) often kills a broad variety of sensitive gut microbes and leads to dysbiosis which warrants the inclusion of pro- and/or prebiotics to repopulate the gut and modulate the gut microbiome.
The following also deserve due thought:
– Overuse of certain medications like proton pump inhibitors and antihistamines
– Poor liver function
– Poor motility
– Digestive disorders
– Poor pancreatic function
– Inflammation in the gut
– Stress
– Environmental toxins
– Dietary choices
Whilst exposure is crucial for immune system maturation, we can’t ignore that nutrition also plays a role.
The importance of individual amino acids to gut function and immunity has become apparent in recent years due to studies that have supplemented amino acids to animals/humans fed:
1) intravenously (total parenteral nutrition – TPN), which demonstrates not only the importance of GALT but also the importance to immune functions beyond the intestine;
2) during weaning, which demonstrates the importance of these amino acids to the normal growth and development of the intestine and GALT; and
3) during infection or chronic inflammation, which has demonstrated the role in regulating inflammation and infectious challenges.
Glutamine is an important energy substrate and precursor for other amino acids and derivatives in immune cells and enterocytes.
In immune cells, particularly lymphocytes, neutrophils and macrophages, glutamine is used rapidly.
In addition to its role as an energy substrate, glutamine is important for intestinal development and function, including maintaining the integrity of the gut barrier, the structure of the intestinal mucosa and redox homeostasis.
Overall, animal studies have shown that glutamine is required to maintain a healthy intestinal mucosa and support several GALT functions during weaning, infection and other intestinal inflammatory states.
Glutamate is thought to modulate the intestinal epithelium. It is thought to play an essential role as an oxidative substrate to both enterocytes and immune cells.
It is also a precursor for the synthesis of GSH (glutathione), which is required to protect the intestinal mucosa and optimise immune cell function.
Finally, glutamate is a precursor for arginine, the substrate for the synthesis of NO. A high rate of NO synthesis by neutrophils is required during the innate immune response to infection which is an important role of the immune system in the intestine.
Studies have shown that arginine supports the growth and the development of the intestine and mucosal barrier in animals.
There is considerable support that in health and stressed conditions, ingestion of arginine has a beneficial effect on GALT, with particular improvements in aspects of the acquired immune response.
Arginine is thought to support the growth, development and maintenance of a healthy intestinal mucosa during critical periods of development and under certain health conditions.
Whilst protein intake is essential to immune function, the availability of specific dietary amino acids, in particular glutamine, glutamate, and arginine, and perhaps others, are essential to optimising the immune functions of the intestine and specific immune cells located in GALT. These amino acids modulate their effects by maintaining the integrity, growth and immune functions of the epithelial cells in the intestine, as well as improve T-cell numbers and function, the secretion of IgA, and regulate inflammatory cytokine secretion.
Sources of Glutamine:
Sources of Glutamate:
Sources of Arginine:
We would always advocate a fresh food diet to provide the nutrients necessary for healthy immune functioning in your pets. If you would like any support in optimising your pet’s health, check out our services to see how we can help.
Thanks for reading,
MPN Team